
Pulsed field ablation could be a preferred initial approach for some patients with a more advanced form of the condition.
A decades-long research journey led by Vancouver Coastal Health Research Institute researcher Dr. Jason Andrade is reshaping how clinicians approach atrial fibrillation (AFib), one of the world’s most common and consequential heart rhythm disorders. Affecting roughly 170,000 British Columbians, AFib is an irregular heartbeat that doubles the risk of death and increases the likelihood of stroke or heart failure five-fold.

Andrade’s recent study, published in The New England Journal of Medicine, focused on patients with a more advanced form of AFib, called persistent AFib: a continuous abnormal heart rhythm lasting more than seven days. Almost all patients with the condition also present with atrial myopathy, a type of heart muscle disease that reduces the heart’s ability to pump blood throughout the body.
Individuals with advanced AFib are inherently different from those with other forms of arrhythmia, tending to have more co-existing health conditions that influence decision-making surrounding treatment, Andrade explains. “AFib is a chronic and progressive disease. While its early forms are characterized by isolated electrical abnormalities, as it progresses, more abnormalities develop in the structure and function of the heart, increasing the risk of complications.”
Expanding arrhythmia treatment options for enhanced patient care
For years, treatment for persistent AFib followed the same path: begin with antiarrhythmic drug therapy and reserve procedures like catheter ablation for when those therapies fail. Andrade’s work is the first to prove the efficacy of catheter ablation as an initial treatment for patients with advanced forms of AFib.
“This is the first large-scale, international randomized clinical trial examining the role of catheter ablation as the initial treatment for persistent AFib, making inroads in informed treatment decision-making.”
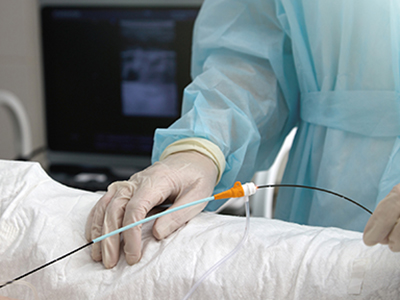
Andrade’s research compared two initial treatment strategies among patients with persistent AFib: antiarrhythmic medications — the longstanding first-line approach — and a new form of minimally invasive catheter ablation called pulsed field ablation (PFA).
Traditionally, ablation has relied on thermal energy using either heat or freezing to disrupt faulty electrical pathways. While effective, these approaches carry risks of damage to surrounding structures, such as the esophagus or nearby nerves. By contrast, PFA uses electrical impulses to selectively target heart tissues, reducing the potential of negative effects.
“Pulsed field ablation is tissue-specific, so more targeted to the tissue we want to affect, with a lower risk of collateral damage.”
In the clinical trial, more than 300 patients with previously untreated persistent AFib were randomly assigned to receive either PFA or drug therapy. All participants were monitored continuously for one year using implantable cardiac devices, allowing researchers to precisely track arrhythmia recurrence.
At 12 months, 56 per cent of patients who received PFA achieved treatment success, compared to just 30 per cent of those on antiarrhythmic medications. Patients in the ablation group also experienced a significantly lower burden of arrhythmia over time.
Findings support informed treatment decision-making for AFib
The findings build on earlier work from Andrade’s team. Around five years ago, their research showed that catheter ablation using freezing energy was more effective than medications in patients with early-stage AFib. A subsequent study demonstrated that early intervention could slow disease progression.
These studies on early-stage AFib led to rapid changes in clinical practice worldwide, with ablation increasingly adopted as a first-line therapy. The new findings suggest similar benefits may extend to patients with more advanced disease.
“Our study demonstrated that catheter ablation using the novel pulse field energy was significantly more effective than using antiarrhythmic drugs as the first-line therapy.”
“We know that early treatment for atrial fibrillation leads to a lower risk of stroke and death,” Andrade says. “The question was how best to provide that treatment. This study helps guide clinicians and patients in making that choice.”


