
Our skin research expert explains the difference between sunburn and sun allergy.
We know that exposure to the sun’s rays can cause premature aging of the skin, but in some cases it can also lead to an allergic reaction. Dr. Harvey Lui explains how to tell if that rash is from the sun and when to see your doctor.
Q: My friend says she is allergic to the sun. Is there such a thing as a sun allergy?
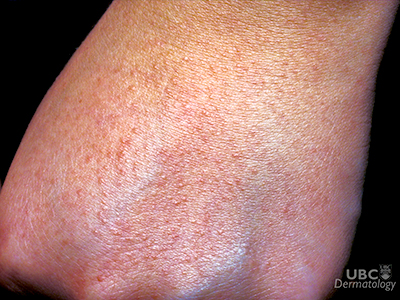
A: Yes, people can develop an allergic reaction to the sun called polymorphic light eruption (PLE). This causes a delayed skin reaction after exposure to ultraviolet (UV) radiation, typically from the sun. People with PLE often experience a rash and itching. This differs from the pain or swelling of sunburn, which can be mistakenly called ‘heat rash’. It is actually sunlight, and not heat, that causes the skin reaction. The best way to know for sure if you have PLE, sunburn or some other type of light sensitivity is to speak with a physician.
Q: What triggers a sun allergy?
A: Each exposure to sunlight can trigger the recurrence of a sun allergy rash, which tends to subside after two to five days. In some cases, it may be a hereditary condition. Research shows that, over time, repeated exposure to UV radiation can cause the body to develop an immune response to the sun, similar to environmental pollen and hay fever. This is because sun exposure can produce changes in skin cells that the body’s immune system may identify as being foreign, or abnormal antigens. In cases of PLE, a rash and itching could be the result of the immune system attacking these antigens. However, a definitive cause of PLE has yet to be identified.
Q: Who is most likely to develop a sun allergy?
A: Sun allergy is a common condition that affects up to 10 per cent of the population. Women and people with fair skin are more prone to PLE, which is most prevalent in regions with distinct seasons, such as northern climates. Countries near the equator have much lower instances of PLE because people there are exposed to higher UV levels year-round. An ongoing exposure to intense sunlight allows them to build up a tolerance to UV radiation, which guards against sun allergies. In places with low UV radiation in the winter, people with PLE tend to have more severe symptoms in the spring. Their symptoms improve in the summer months as they become more tolerant to UV exposure.
Q: How is a sun allergy treated?
A: The best defense against PLE is to block as much sunlight from reaching the skin’s surface as possible to prevent the return of symptoms. Patients are advised to cover up with clothing and wear sunglasses and a hat. It is also recommended to use a broad spectrum sunscreen with an SPF (sun protection factor) of at least 30, but ideally 60 or higher.
To help relieve the itchy rash caused by PLE, apply cortisone creams or ointments. In more severe cases, patients may be referred to our Phototherapy Clinic at the Vancouver General Hospital Skin Care Centre for desensitization or light-hardening treatments. We expose patients to prescribed low doses of UV radiation on a regular basis using our UV phototherapy unit. After time, this procedure can be effective at reducing the occurrence and symptoms of PLE.



