
TEE Shuttle protects echocardiogram probes from contamination and saves money.
Senior biomedical engineer technologist Daniel Driedger’s original motivation for gathering feedback from six stakeholder groups at Vancouver General Hospital (VGH) and advice from more than 20 medical professionals about how to better handle and transport a commonly used cardiac surgery device was simple: cost savings. The device, known as a transesophageal echocardiogram probe (or TEE probe), uses an ultrasound transducer at its tip that, when inserted into the esophagus during an echocardiogram, records images and offers Doppler evaluation during cardiac surgery procedures. Driedger and his colleagues tracked a high frequency of costly TEE probe repairs over several years and found that a proper, standardized, process for taking care of the device was necessary but non-existent.

“As I learned more about the use-cycle of the TEE probe, an opportunity presented itself to develop its own standard of care in terms of handling, transportation, and storage,” says Driedger, who works in VGH’s Biomedical Engineering Department and is also the Safety and Technical Coordinator, Hyperbaric Oxygen Therapy, at VGH. “Due to its unusual configuration and delicate nature, the TEE probe didn’t follow a normal workflow pathway; it was a phantom device with no dedicated solution to containerize before or after use.”
TEE probes, by design, require two different levels of cleaning: manual intermediate-level disinfection for the non-patient parts and processing in an automated TEE disinfection machine for high-level disinfection of the patient part. Probe replacement costs range from $20,000 to $80,000, and repair costs start at $5,000.
By seeking advice and expertise from anesthetists, anesthesia assistants, operating room nurses, device reprocessing staff, infection control employees, biomedical engineers, product designers and fabricators, among others, Driedger was able to design the TEE Shuttle - an apparatus that complies with standards and best practices.
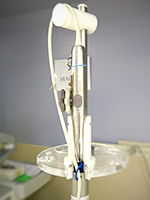
Designed to accommodate both cleaning levels, the TEE Shuttle incorporates two overlapping crescent tubes, which allows the patient part of the TEE probe to be contained and protected after disinfection. The uniquely shaped crescent tubes, assembled with end caps to form the shuttle, allow the unit to be docked onto a roll-stand. This allows for safer transportation and storage of the TEE probe and improved ergonomics to access the TEE probe in the procedure room.
“The TEE Shuttle truly reflects inter-professional collaboration and innovation within our community,” says Driedger, who spent five years moving from concept, prototype, trials and implementation, to development of the apparatus.
“Historically, physicians needed to retrieve the TEE probe from outside the operating room, mid-procedure. The Tee Shuttle allows them to bring the device in beforehand, improving work-flow during critical parts of the procedure.”
Currently, the TEE Shuttle is being used in the cardiac surgical operating rooms at VGH. Driedger plans to introduce it to other sites within the region. Since the TEE Shuttle was introduced three years ago, Driedger and his colleagues have noted a significant reduction in repair costs.

“Feedback has been extremely positive,” Driedger notes. “In particular, physicians indicate that the shuttle has become a normal part of the TEE patient procedure.”


