
The naturally occurring molecule has been proven to combat lung infections and support healthy lung function.
When the COVID-19 pandemic struck, Dr. Jeremy Road and colleague, Dr. Chris Miller, recognized that their work with nitric oxide could be a game-changer. They were in the midst of examining the application of the virus-, bacteria- and fungus-killing free radical against non-tuberculous mycobacterial and other infections, and quickly pivoted their investigations towards the new coronavirus.
“Based on our knowledge and experience using nitric oxide to treat other lung infections, we believe it could prevent COVID-19 infections from progressing and ultimately improve outcomes for patients, particularly more vulnerable patients,” says Road, a Vancouver Coastal Health Research Institute (VCHRI) researcher.
“COVID-19 allowed us to focus on the potential application of the virus-destroying properties of nitric oxide.”
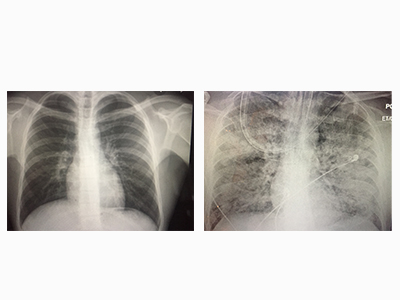
There is presently no vaccine or cure for COVID-19. While most individuals will recover from the disease, seniors and people with compromised immune systems are at greatest risk of hospitalization. In severe cases, COVID-19 can lead to acute respiratory distress syndrome (ARDS)—when a buildup of fluid in air sacs in the lungs deprives the body of oxygen, causing severe illness and potentially death.
Nitric oxide is a free radical molecule that is naturally produced by cells in the body to stabilize blood flow and blood pressure. It also fends off infection when released by the immune systems’ white blood cells, and destroys microorganisms and viruses on contact.
Road and colleagues are researching the clinical outcomes of administering nitric oxide gas at a concentration of 160 parts per million to patients with COVID-19, non-tuberculous mycobacteria, aspergillus or burkholderia lung infections. The research team will assess whether nitric oxide can reduce the viral and bacterial load in the lungs, improve patients’ breathing and reduce the need for oxygenation and ventilation.
“This study could be a game changer in restoring normalcy in the COVID-19 era prior to an effective vaccine.”
The upper airway is the predominant gateway for COVID-19 to entre into the body. Once inside, the virus binds to cells, multiplies and bursts cells, shedding tens of millions of virus particles into the airway. These virions then reach the lungs where they can cause a deadly inflammatory process that leads to ARDS. When nitric oxide is administered to patients infected with COVID-19, it has the potential to decrease the viral load, along with inflammation caused by the body’s immune response.

“Ideally, the treatment would be introduced during the early stages of a COVID-19 infection,” says Road. “However, nitric oxide may also help patients in later-stage disease progression.”
A ray of hope for difficult to treat infections
Nitric oxide has some clinical applications already, including in the treatment of pulmonary hypertension. It can also destroy a wide variety of microbes that lead to non-tuberculous lung disease caused by mycobacteria.
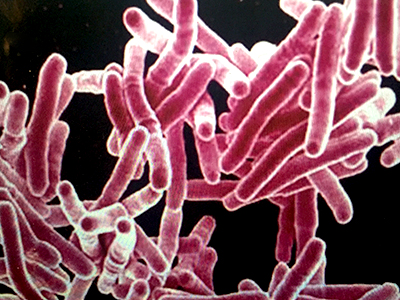
Exposure to any of the around 140 species of mycobacteria found in nature is often inconsequential. However, these microorganisms can give rise to a debilitating infection among some individuals with compromised immune systems, as well as the elderly.
With rates of mycobacterial infection on the rise1—and a growing concern about several that have developed antibiotic-resistance—the clinical application of nitric oxide is part of a new line of research into novel treatment options for this patient population.

Road, Miller and colleagues’ preliminary research has shown that, when administered at the correct concentration, nitric oxide is a potent anti-microbial agent against mycobacteria that can help reduce bacterial load and rein in disease proliferation.
So far, their clinical results show the safety of inhaling 160 parts per million of nitric oxide for up to 80 minutes. One patient has used it daily for over two years, says Road. Data also show that, as drug resistant bacterial loads decrease, patients’ energy and quality of life increases.
“With more people reaching elderly ages, and more immunocompromised patients, there is a need for better treatment options for mycobacterial infections,” says Road. “The results of our research will uncover more clues about how to optimally apply nitric oxide for better treatment outcomes for patients.”


