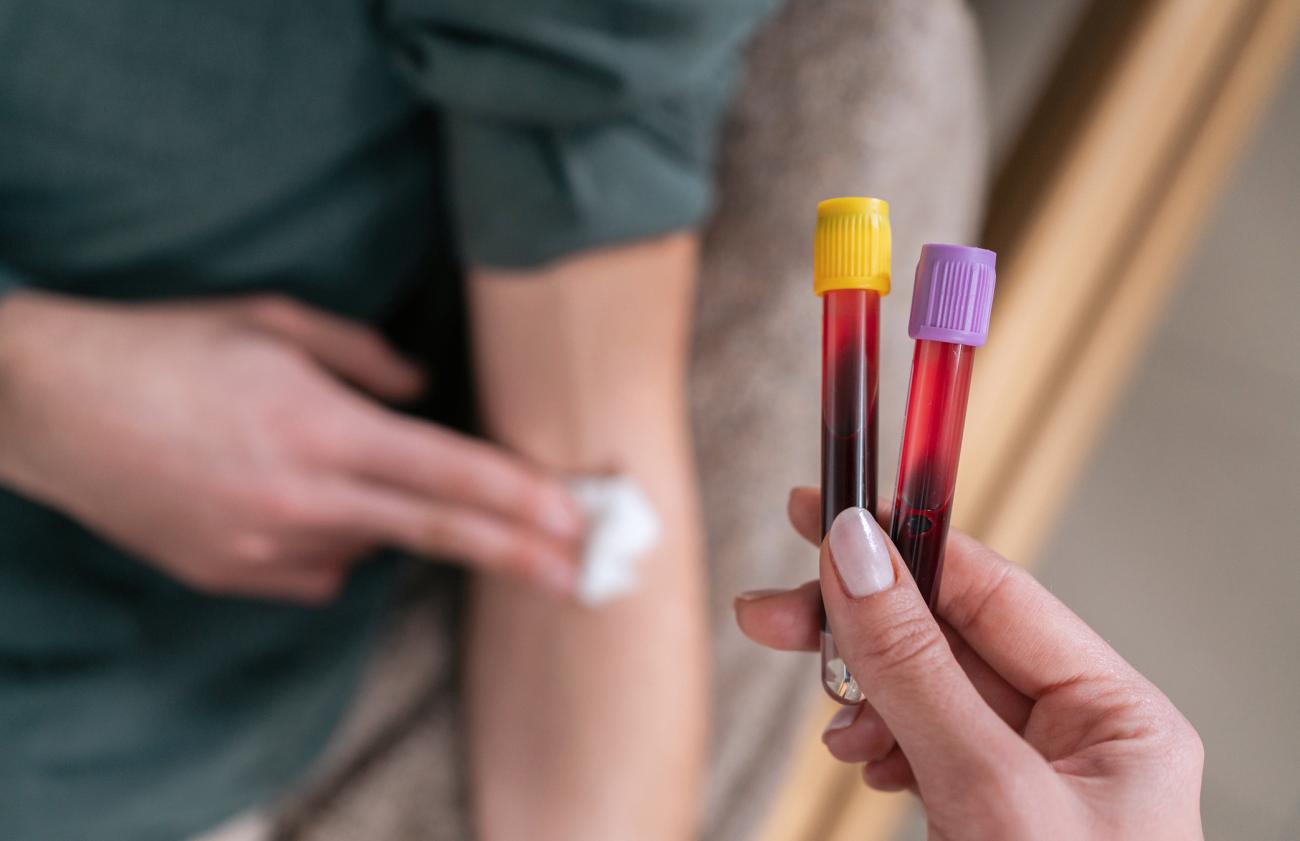
Research into the triple bottom line of sustainable health care uncovers new ways to reduce costs to people, health care and the environment.
Climate change is a universal problem that impacts both environmental and human health. In response, Vancouver Coastal Health Research Institute researcher Dr. Andrea MacNeill and Dr. Karina Spoyalo are looking at how sustainable health care can contribute to reducing greenhouse gas emissions and mitigate the harms associated with climate change.

“One of the biggest takeaways in the emerging field of sustainable health care is that what is good for the environment is good for patients,” states Spoyalo. “The sum of the parts becomes greater in the end.”
“Globally, health care contributes 5.2 per cent of greenhouse gas emissions. In Canada, pollution from the health care industry accounts for 23,000 disability-adjusted life-years lost annually.”
In her 2021 research paper, MacNeill defines a framework for constructing the emerging field of environmentally sustainable health systems. She describes it as reducing the demand for health services through preventive measures; avoiding unnecessary investigations and treatments; and decarbonizing processes of care.
“The health sector is uniquely positioned to lead global climate action,” states MacNeill. “Rethinking health care through a holistic lens of sustainability will help realise the Canadian federal government’s goals of achieving net zero emissions by 2050 and developing low-carbon, sustainable and resilient health systems.”
A call for reducing unnecessary blood work
MacNeill and Spoyalo’s recent study, published in BMJ Open Quality, applies a triple bottom line framework that estimates the burden of unnecessary blood work on acute care surgical patients. The triple bottom line approach is used to assess treatment outcomes in terms of impacts to patient health, health care expenditures and the environment.
The research team looked at the hospital records of 304 patients admitted to hospital with a handful of acute yet uncomplicated conditions. Of these, 83 patients were randomly selected for an in-depth chart review.

The team compared the blood work requested in the studied cohort against recommendations for appropriate investigations that were agreed upon by 17 general surgeons at VGH. They found that 76 per cent of the patients reviewed in-depth underwent unnecessary blood work.
Researchers found that the unnecessary blood work ordered contributed to a mean 1.84 additional requisitioned blood draws, 16.5 blood tests — individual tests that pathologists conduct on blood draws — and 18 millilitres of blood per patient. This resulted in $5,235 of additional costs from the health care system and an extra 61 kilograms of greenhouse gas emissions known to contribute to climate change.
“Similar to the campaign to stop the misuse of antibiotic medications, we need to educate health care providers about why appropriate testing is better than more testing.”
However, getting to the stage of promoting smarter testing first requires a body of evidence to back up triple bottom line recommendations, adds Spoyalo. “You cannot fix or improve something that you do not fully understand.”
“We are now learning a lot more about the potentially harmful effects of unnecessary testing, such as blood work.”
“What we need now is thoughtful ordering of laboratory investigations,” says Spoyalo. “This could include unbundling blood tests to avoid wastage, as well as educating physicians and patients about the costs and human and environmental harms associated with unnecessary lab work.”


