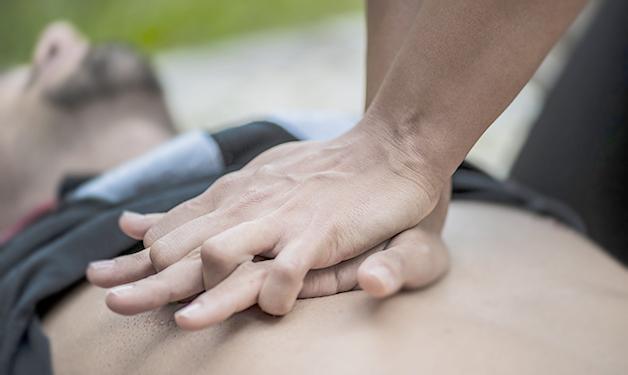
Recent study finds patients who received temperature management sooner after hospital admission were more likely to survive.
Walking the halls of the emergency department as a cardiology fellow, Dr. Christopher Fordyce saw how some cardiac arrest patients waited longer than others to receive an essential cooling treatment. It occurred to Fordyce, who is now a cardiologist at Vancouver General Hospital (VGH) and a Vancouver Coastal Health Research Institute researcher, that the varying times before a cooling treatment was administered might impact patients’ health outcomes.

“There were many reasons to delay the administration of cooling treatments, such as waiting until a patient arrived in the coronary care unit or received a coronary angiogram,” says Fordyce, “but I wanted to know if that wait time had an impact on a patient’s survival and neurological health.”
Fordyce’s research paper—published in the Journal of the American Heart Association around six years after he first conceived of his research question—delivers statistical evidence to support the early administration of cooling methods after a patient arrives in hospital with cardiac arrest.
“Up to now there has been a lack of urgency to create strict guidelines around the timing of cooling interventions, despite the fact that they can improve patient outcomes.”
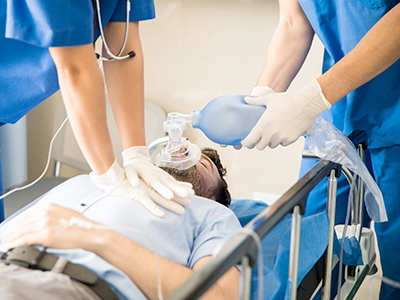
Targeted temperature management (TTM)—formerly called therapeutic hypothermia—is the intervention used to cool down the body temperature of cardiac arrest patients when they arrive in hospital. The treatment can be administered externally using ice packs and cooling blankets, and internally using cold IV fluids and endovascular methods to deliver cooling liquids into the bloodstream.
The end goal of TTM is to bring a patient’s body temperature down to around 33-36 degrees Celsius1. This temperature reduces damage to tissues, including the brain, caused by cardiac arrest and the heart being unable to effectively pump blood throughout the body.
Fordyce’s study is the first to examine the time it took for cardiac arrest patients to receive TTM after arriving through the doors of a hospital, called door-to-TTM (DTT).
Intervening with cooling earlier resulted in less neurological damage for some patients
The statistical information used in Fordyce’s study came from the Continuous Chest Compressions trial in British Columbia. Of the 3,805 patients included in the trial, 570 met the eligibility criteria examined by Fordyce’s team.
Researchers found that the median time to receive cooling in the early DTT group of patients was 35 minutes. In the late DTT group, it took 218 minutes to receive a cooling treatment—over six times longer.
“The study’s results clearly show that early DTT increased the likelihood that patients would leave the hospital alive.”
This not only benefits patients, notes Fordyce, it can also avert the need for additional health care resources for treatments, and potential long-term care for patients with severe neurological damage.
“Early administration of TTM may not be the only reason for these positive results,” cautions Fordyce. “Other things like the bundle of care provided to patients, including blood pressure and oxygenation targeting and cardiac interventions must also be factored into the bigger picture of survival rates. However, we can say that an hour or two delay before TTM is administered can make a difference in patient outcomes.”
“TTM is not new; it is a standard of care. What these study results indicate is that we should be delivering the treatment sooner rather than later.”
Fordyce is working to raise awareness about the results of his study and how to implement protocols to ensure that cardiac arrest patients who present to hospital receive cooling treatments as soon as possible. He was awarded a Physician Led Quality Improvement Project through Vancouver Coastal Health to support his efforts to reduce DTT time at VGH.
“At the end of the day, patients care most about survival and avoiding brain damage,” says Fordyce. “This research shows that earlier cooling interventions can help deliver better outcomes in these two areas.”
1 BC Emergency Medicine Network - Post Cardiac Arrest: Targeted Temperature Management (TTM)


