
A therapy that involves family generated iPad videos for patients with dementia expands its reach with an online toolkit.
A care intervention that connects people with dementia to loved ones via pre-recorded videos is being expanded to a global audience. The online toolkit for the iPad Simulated Presence Therapy—developed by Vancouver Coastal Health Research Institute researcher Dr. Lillian Hung and her research team—explains how to enhance the care and quality of life of people living with dementia with videos created by their loved ones.

“By making this toolkit available online, we can assist hospitals and care facilities around the world with implementing portable video technology for people with cognitive impairment,” says Hung.
“The use of family generated videos strengthens personal connections between people living with dementia and their family members.”
The toolkit includes videos that describe the family, patient and staff experience, as well as advice on how to create short, positive and encouraging videos of loved ones. It also features a downloadable brochure with information about the therapy for family members and a pocket card for health care staff.
In this patient experience video, Mario, a person living with dementia, explains the hospital environment experience and the comfort iPad therapy can provide to patients:
Currently offered to patients with cognitive impairment at Richmond Hospital and Vancouver General Hospital (VGH), the video therapy recently received an upgrade in the form of a first-of-its-kind lockbox and articulating arm on wheels. The portable iPad mounting system, developed by the Biomedical Engineering Department at VGH, secures the password-protected iPads and makes it easier for clinicians to safely angle them into an optimal viewing position for patients.
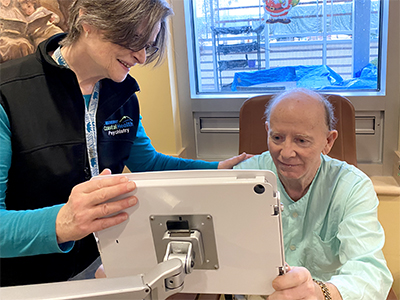
“The iPads also have other uses outside of the family videos, such as: to play music and movies for patients, and to provide information in the patient’s preferred language,” says Hung. “At Richmond Hospital, staff and the son of a female patient used the iPad to find one of her favourite songs from Japan.”
A person-centred approach to dementia care
Memory loss and declines in cognitive abilities are the hallmarks of dementia, which can lead to confusion and disorientation, along with lashing out. Around 62,000 British Columbians have the condition, which mostly affects adults over age 65. That number is expected to rise to 87,000 residents by 20241.

In a needs assessment conducted by Hung and colleagues in 2017, nurses at VGH identified caring for people with dementia as the most challenging aspect of their work. Nurses mentioned being fearful of interacting with patients with dementia who might be prone to violence, such as kicking and punching.
“These kinds of incidents are distressing for the care provider and care facility, as well as for the patient and his or her family members,” says Hung.
Showing people with dementia short—around one-minute—pre-recorded videos in which a loved one explains a course of care, such as administering medication or a bathing routine, is often the reassurance they need. When patients with dementia understand what a care provider is trying to do, they often calm down and cooperate. The videos can also sidestep the need to use sedatives or restraints to protect the patient and care providers from injury.
“People with dementia may not recognize where they are or their care providers, but they often find reassurance in seeing and hearing loved ones.”
For example, a patient who missed his wife was shown a video of her wearing a pendant he gave her during their initial courtship. She tells him that she loves him and that he is okay at the hospital. The video alleviates the patient’s fear that he had been abandoned, says Hung.
“Videos like this can be shown to patients throughout the day to help them calm down and feel safe and comforted.”
Not only is this a benefit to patients and their family members, says Hung, “staff members at Richmond Hospital and VGH also report that the iPad has become a useful tool they routinely access during their day for dementia care.”
Learn more about the iPad project for people with dementia and access the toolkit online.
The iPad project research team consists of patient partners (Mario Gregorio, Jim Mann), family partners (Annette Berndt, Christine Wallsworth, Neil Horne), physicians (Bryan Chow, Ryan O’Neill) and nurses (Cheryl Chan, Cathy Son).


