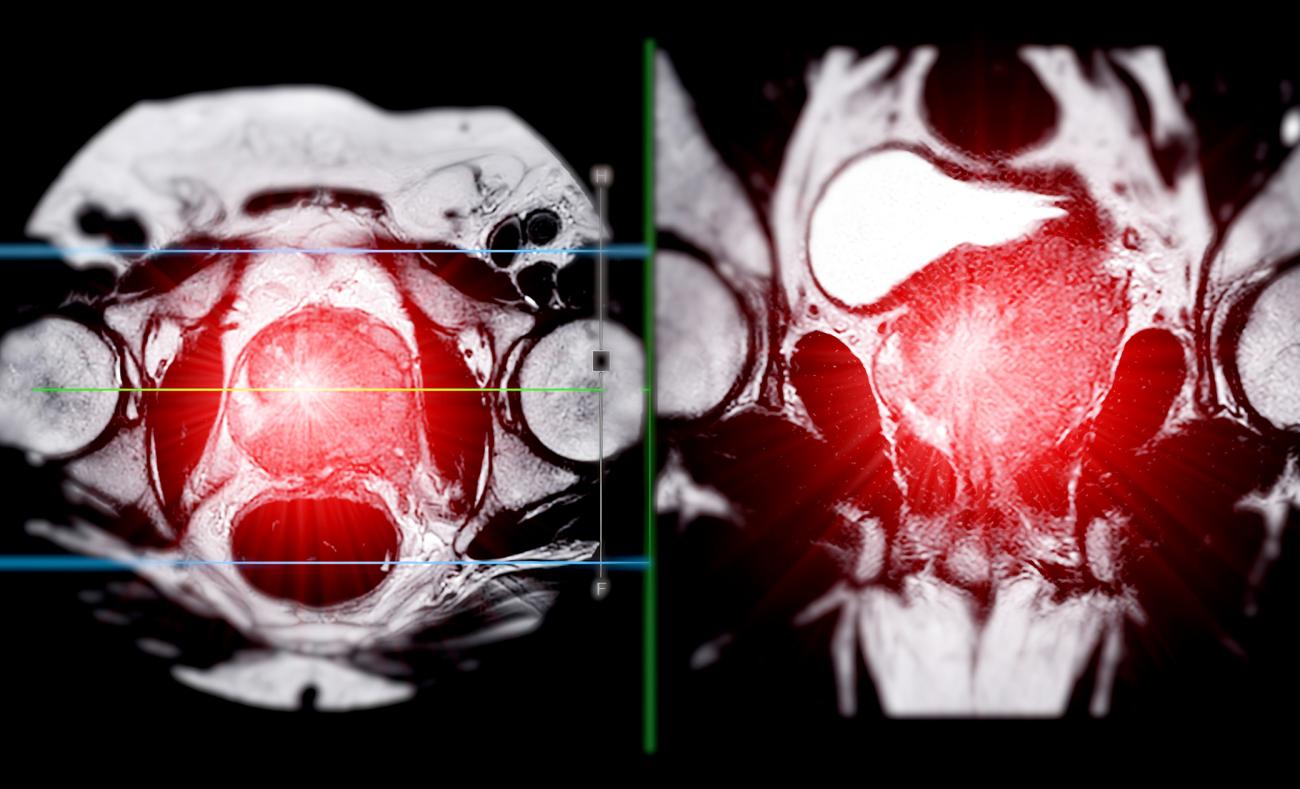
Resolving the paradox of UGT2B17 adds fuel to the fire of ongoing targeted medication research.
Scientists have discovered additional functions of a protein involved in the underlying mechanisms of metastatic prostate cancer, expanding the understanding of potential treatment pathways for the disease. Led by Vancouver Coastal Health Research Institute researcher Dr. Xuesen Dong and published in The Journal of Clinical Investigation and European Urology Oncology, the findings are the first to identify other functions of the UDP-glucuronosyltransferase 2b17 (UGT2B17) beyond its enzymatic activity.
“UGT2B17 has been a dilemma,” shares Dong. “It is understood to perform the function of destroying androgen hormones that drive prostate cancer; however, it was also found to be significantly elevated in treatment-resistant tumours.”

Prostate cancer is driven by androgens, which are male sex hormones, such as testosterone. The first-line treatment for prostate cancer is androgen deprivation therapy, designed to block androgen production in the body.
Approximately 30,400 Canadians are diagnosed with prostate cancer each year, with the vast majority of patients responding well to front-line therapies early in the disease progression. However, with time, most prostate cancers stop responding to androgen deprivation therapy and become treatment resistant.
Enzyme interacts with two other proteins to potentially drive cancer growth
To explain the paradox of elevated levels of the androgen-reducing UGT2B17 in metastatic prostate cancer, Dong and his team’s analysis targeted the enzyme, which is a type of protein, using mass spectrometry-based proteomics. Mass spectrometry is a specialized approach to determine the weight of molecules in a sample, with proteomics geared specifically toward profiling proteins, their interactions and modifications, and how they affect cell function in the body.
“UGT2B17 enables prostate cancer cells to withstand androgen deprivation therapy-induced stress and continue proliferating through mechanisms that are independent of its enzymatic activity.”
Dong’s analysis of UGT2B17 — which included large, multi-institutional Canadian cohorts — focused on characterizing other mechanisms that the enzyme performed in the body other than eradicating androgen hormones, which is UGT2B17’s enzymatic activity. The team’s investigation resulted in the discovery of significant interactions between UGT2B17 and two other cancer-associated oncogene proteins: protein disulfide isomerase (PDI) and Src kinase.
“Src is already a well-known medication target for leukemia, a cancer of the blood and bone marrow, and PDI is known for promoting tumour growth,” says Dong, adding that both PDI and Src are also therapeutic targets for several other cancers, including breast and ovarian cancers. “However, UGT2B17 was interacting with these other proteins in very different ways.”
UGT2B17 contributes to the production of Src, which acts as an androgen receptor in the absence of androgens to promote prostate cancer growth. On the other hand, UGT2B17 modulates the prevalence of PDI. Because PDI supports the proper folding of proteins in cancer cells, its functioning can determine cell survival or death.
“What we found was that UGT2B17 performs an imperative role in metastatic prostate cancer functions that likely contribute to cancer cell survival and proliferation.”
The newly discovered functions of UGT2B17 underscore its significant downstream effects on PDI and Src. However, as blocking UGT2B17 can lead to serious liver damage, additional investigations are necessary to define the enzyme and its functions.
Looking ahead, Dong sees the interconnected relationship between UGT2B17, PDI and Src as a promising avenue of research to explore, with the long-term goal of achieving further advances in metastatic prostate cancer treatments.


